Mothers, retirees, veterans, scientists, and working-class Americans sent letters by the dozens over several months to the commission formed this year by Donald Trump to help solve the opioid crisis. One concern united them: Tight restrictions on prescription pills could be driving pain patients to turn to heroin and fentanyl.“If the U.S. government is to deal with the opioid epidemic, the first thing you must realize is that managed prescriptions to chronic pain patients didn’t cause the problem,” wrote one such patient from Kalispell, Montana. “And torturing us by denial of care will only make the mess worse when we must go into the street to get pain relief.”And yet, 25 of the 56 recommendations included in the commission’s final report, released last week, call for a continued crackdown on prescription opioids and other “supply reduction and enforcement strategies.” At the same time, the report acknowledged that these policies likely contributed to the massive spike in fatal overdoses in recent years. It’s as if the commission, led by New Jersey Gov. Chris Christie, believes Trump can double down on an approach that made the problem worse and it will somehow produce a different result.“This is a giant show of what is quickly doable, but it has no medical-outcome data to support it,” said Stefan Kertesz, a professor of preventive medicine at the University of Alabama at Birmingham. “There’s no evidence you stop overdoses by taking patients off opioids against their will. Moreover, that course of action frequently destabilizes patients who are being taken off of them.”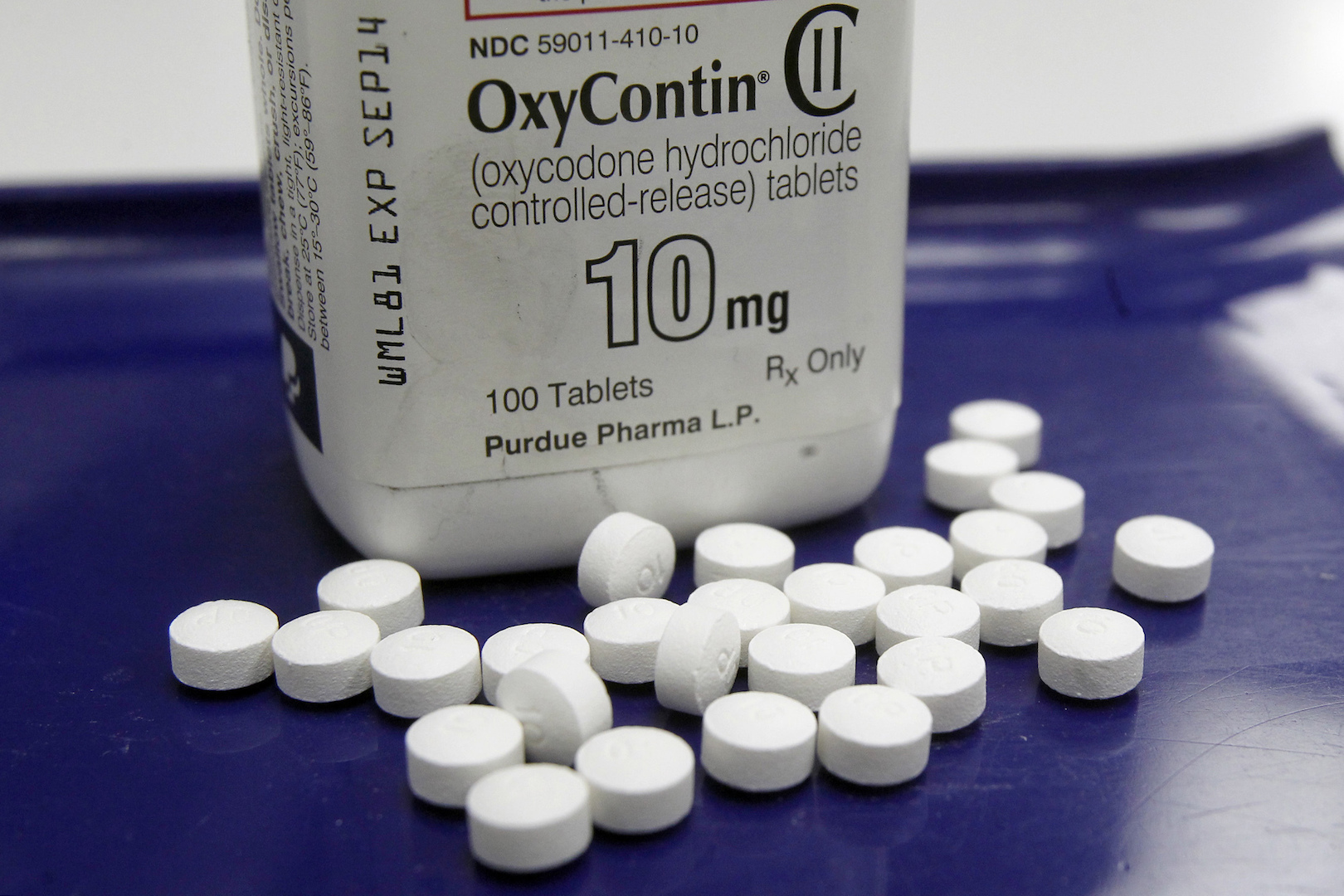 READ: How the maker of Oxycontin tried to influence Trump’s opioid commissionAmerican pharmacies still dispense three times as many opioids as they did in 1999, but prescribing rates have been falling steadily since 2011, due in large part to CDC guidelines that discourage primary care doctors from putting patients on opioids for pain that lasts longer than three months. Even so, government officials remain fixated on painkillers. At least 17 states have limited doses or prescription durations. Attorney General Jeff Sessions also created a special Department of Justice unit to investigate doctors and pharmacists suspected of illegally dispensing painkillers.It’s true that a glut of powerful painkillers flooding the market helped trigger the opioid epidemic, but the latest data — including stats cited by Christie’s commission — show that the problem has since metastasized. The commission’s report includes a remarkable section under the heading “lack of foresight of unintended consequences,” which notes that as painkillers became more scarce, “market forces responded” by supplying cheap, powerful, and deadly synthetic opioids like fentanyl.“Black market heroin is currently much less expensive than diverted prescription opioids, and fentanyl is even much less expensive per dose than heroin,” the report states. “Predictable from the economics of the two drug categories, the prescription drug overdose problem has decreased, but not the overall number of opioid-related deaths.”“You get some patients who have become either physically dependent or addicted, turning to what they can buy on the street, either diverted opioids or illicit opioids,” Christie spokesman Brian Murray told VICE News. “The report has several recommendations that speak to physicians’ need to understand and screen for addiction, so they don’t cut off an addict without an appropriate tapering protocol and/or helping that person get into a treatment program.”The letters sent to Trump’s commission, obtained by VICE News using the Freedom of Information Act, reveal the desperate situations pain patients find themselves in when they abruptly lose access to medication.“I lost my life. I would like it back, please,” wrote one woman from Kentucky, who described having back pain and other problems. “I can not keep waking up every day to pain and living through moments of a bit of lower pain but still stuck on my couch. Please let me live!”For doctors like Kertesz, the situation is maddening. He hears about suicides on a near-weekly basis by patients who have lost access to painkillers, and he says recent anti-opioid prescription policies have “incentivized abandonment” of pain patients.“There has been a tremendous expectation that reductions in opioid prescribing for pain is going to reduce or eliminate or resolve much of this problem,” Kertesz said. “I agree that excessive prescribing played a role in unleashing this problem, but the issue is not perfectly symmetrical. If you stick a fork into an electrical outlet and get shocked, the solution is to remove it. We’re all hoping this a fork-removal problem. That’s a false hope.”
READ: How the maker of Oxycontin tried to influence Trump’s opioid commissionAmerican pharmacies still dispense three times as many opioids as they did in 1999, but prescribing rates have been falling steadily since 2011, due in large part to CDC guidelines that discourage primary care doctors from putting patients on opioids for pain that lasts longer than three months. Even so, government officials remain fixated on painkillers. At least 17 states have limited doses or prescription durations. Attorney General Jeff Sessions also created a special Department of Justice unit to investigate doctors and pharmacists suspected of illegally dispensing painkillers.It’s true that a glut of powerful painkillers flooding the market helped trigger the opioid epidemic, but the latest data — including stats cited by Christie’s commission — show that the problem has since metastasized. The commission’s report includes a remarkable section under the heading “lack of foresight of unintended consequences,” which notes that as painkillers became more scarce, “market forces responded” by supplying cheap, powerful, and deadly synthetic opioids like fentanyl.“Black market heroin is currently much less expensive than diverted prescription opioids, and fentanyl is even much less expensive per dose than heroin,” the report states. “Predictable from the economics of the two drug categories, the prescription drug overdose problem has decreased, but not the overall number of opioid-related deaths.”“You get some patients who have become either physically dependent or addicted, turning to what they can buy on the street, either diverted opioids or illicit opioids,” Christie spokesman Brian Murray told VICE News. “The report has several recommendations that speak to physicians’ need to understand and screen for addiction, so they don’t cut off an addict without an appropriate tapering protocol and/or helping that person get into a treatment program.”The letters sent to Trump’s commission, obtained by VICE News using the Freedom of Information Act, reveal the desperate situations pain patients find themselves in when they abruptly lose access to medication.“I lost my life. I would like it back, please,” wrote one woman from Kentucky, who described having back pain and other problems. “I can not keep waking up every day to pain and living through moments of a bit of lower pain but still stuck on my couch. Please let me live!”For doctors like Kertesz, the situation is maddening. He hears about suicides on a near-weekly basis by patients who have lost access to painkillers, and he says recent anti-opioid prescription policies have “incentivized abandonment” of pain patients.“There has been a tremendous expectation that reductions in opioid prescribing for pain is going to reduce or eliminate or resolve much of this problem,” Kertesz said. “I agree that excessive prescribing played a role in unleashing this problem, but the issue is not perfectly symmetrical. If you stick a fork into an electrical outlet and get shocked, the solution is to remove it. We’re all hoping this a fork-removal problem. That’s a false hope.”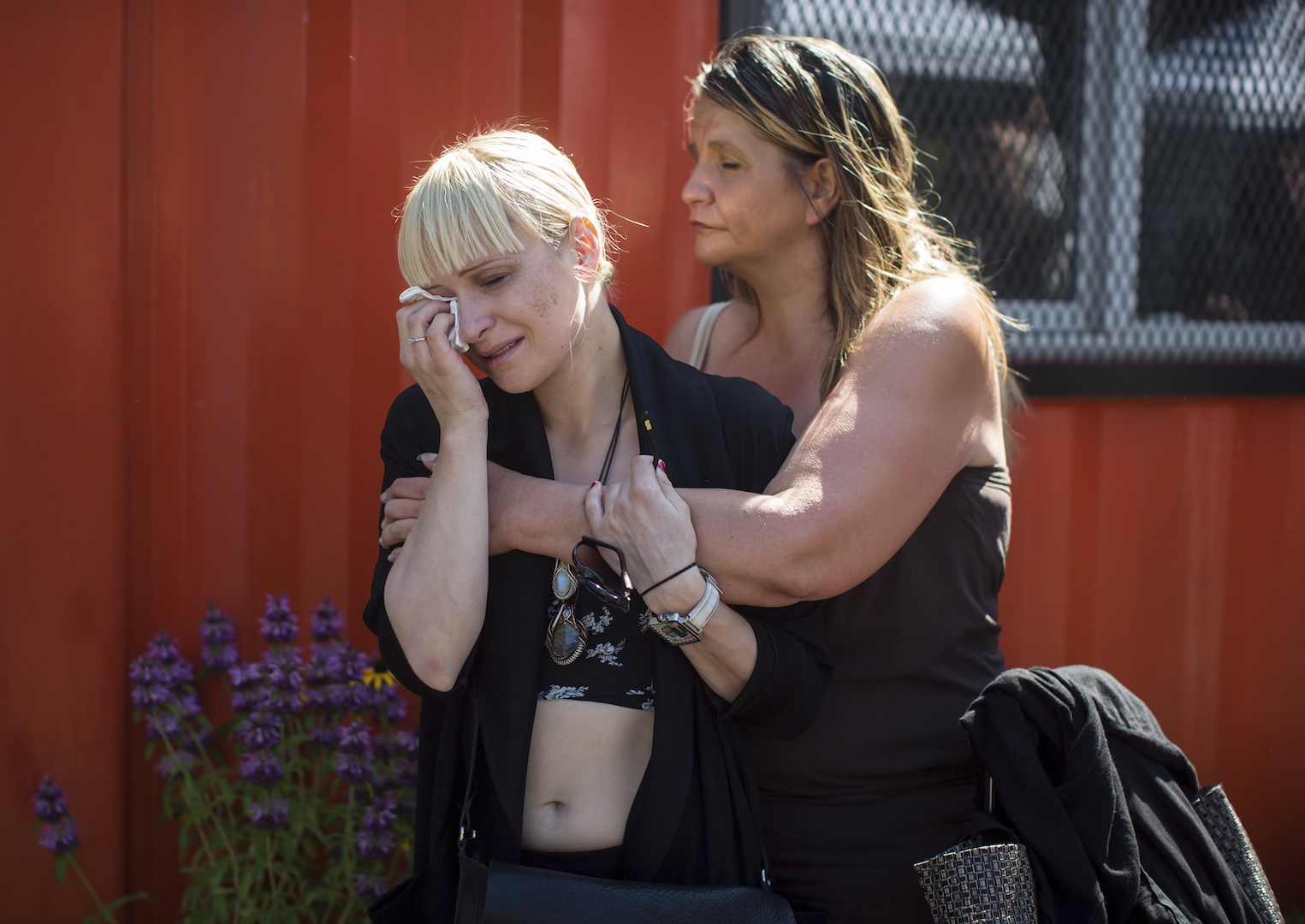 READ: How to get a baby — and a mom — off heroinKertesz has asked the CDC to investigate deaths linked to pain patients losing access to medicine, and he wants policymakers to recognize that the solution to the opioid epidemic is more complex than just reducing the supply of painkillers.A CDC spokesperson acknowledged that chronic pain can increase the likelihood of suicide but that additional research is necessary. Still, the organization aims to “ensure patients have access to safer, more effective treatment individualized to their circumstances,” the spokesperson said. “Clinicians have a responsibility to carefully manage opioid therapy and not abandon patients in chronic pain.” The CDC also noted that heroin use is increasing everywhere, not just areas where opioid prescriptions are decreasing.Among those trying to make the case that the prescription opioid clampdown is claiming lives — not saving them — is Joel Bomgar, a state representative from Mississippi and vice chairman of his Legislature’s Medicaid committee. According to his analysis of CDC data, pill restrictions caused the rate of prescription opioid overdose deaths to fall while fatalities caused by illicit opioid have skyrocketed.“In short, one fewer person per 100,000 is dying from prescription opioids, but we are now killing nearly four additional people per 100,000 from heroin and fentanyl,” Bomgar said. “How’s that for a policy backfiring?”Even among independent experts, there’s no consensus about how exactly the crackdown on prescription opioids is linked to the surge in deaths from fentanyl and heroin. Caleb Alexander, co-director of the Center for Drug Safety and Effectiveness at the Johns Hopkins Bloomberg School of Public Health, believes there’s “a complex, nuanced relationship” between painkiller restrictions and fatal overdoses.“These are in some ways separate epidemics, but in many ways they are two sides of the same coin,” Alexander said. “Some have argued that we’re seeing more people dying from heroin and fentanyl because we’re cracking down on prescription opioids. That’s an erroneous and an overly simplistic read on the evidence.”The dramatic rise in opioid prescriptions can be traced back to 1996, when the American Pain Society launched its influential “fifth vital sign” campaign, which urged doctors to ask patients about pain in addition to checking their blood pressure, pulse, body temperature, and rate of breathing. OxyContin debuted that same year, and manufacturer Purdue Pharma starting marketing the powerful pills to doctors as a relatively safe option for pain patients.
READ: How to get a baby — and a mom — off heroinKertesz has asked the CDC to investigate deaths linked to pain patients losing access to medicine, and he wants policymakers to recognize that the solution to the opioid epidemic is more complex than just reducing the supply of painkillers.A CDC spokesperson acknowledged that chronic pain can increase the likelihood of suicide but that additional research is necessary. Still, the organization aims to “ensure patients have access to safer, more effective treatment individualized to their circumstances,” the spokesperson said. “Clinicians have a responsibility to carefully manage opioid therapy and not abandon patients in chronic pain.” The CDC also noted that heroin use is increasing everywhere, not just areas where opioid prescriptions are decreasing.Among those trying to make the case that the prescription opioid clampdown is claiming lives — not saving them — is Joel Bomgar, a state representative from Mississippi and vice chairman of his Legislature’s Medicaid committee. According to his analysis of CDC data, pill restrictions caused the rate of prescription opioid overdose deaths to fall while fatalities caused by illicit opioid have skyrocketed.“In short, one fewer person per 100,000 is dying from prescription opioids, but we are now killing nearly four additional people per 100,000 from heroin and fentanyl,” Bomgar said. “How’s that for a policy backfiring?”Even among independent experts, there’s no consensus about how exactly the crackdown on prescription opioids is linked to the surge in deaths from fentanyl and heroin. Caleb Alexander, co-director of the Center for Drug Safety and Effectiveness at the Johns Hopkins Bloomberg School of Public Health, believes there’s “a complex, nuanced relationship” between painkiller restrictions and fatal overdoses.“These are in some ways separate epidemics, but in many ways they are two sides of the same coin,” Alexander said. “Some have argued that we’re seeing more people dying from heroin and fentanyl because we’re cracking down on prescription opioids. That’s an erroneous and an overly simplistic read on the evidence.”The dramatic rise in opioid prescriptions can be traced back to 1996, when the American Pain Society launched its influential “fifth vital sign” campaign, which urged doctors to ask patients about pain in addition to checking their blood pressure, pulse, body temperature, and rate of breathing. OxyContin debuted that same year, and manufacturer Purdue Pharma starting marketing the powerful pills to doctors as a relatively safe option for pain patients.
Advertisement

Advertisement
Heroin and fentanyl now account for more than half of the overdose deaths in 10 states, according to the Centers for Disease Control and Prevention. The 2016 National Survey on Drug Use and Health found that 62 percent of adults who misused opioids did so without a prescription, and 40 percent obtained painkillers from friends or relatives, not a doctor. Another study from earlier this year found that heroin now appears to be the most common type of opioid tried by first-time users.“This is a giant show of what is quickly doable, but it has no medical-outcome data to support it.”
Advertisement
Advertisement
Advertisement
In its final report, the opioid commission called for the Centers for Medicare and Medicaid Services to eliminate questions about pain levels from patient satisfaction surveys, but it didn’t stop there. The commission also recommends new training and oversight for opioid prescribers and pharmacists and increase access to addiction treatment but asks Trump to back legislation that would require states to comply with regulations for prescription drug monitoring programs to receive grant money and share prescription data with the Justice Department.In addition to the dozens of pain patients who wrote in to the commission clearly hoping for a better solution, doctors and public health experts also pleaded for a new approach.In one letter, Elizabeth Salisbury-Afshar, a medical director of behavioral health at the Chicago Department of Public Health, warned about the overemphasis on prescription drugs. She noted that painkillers caused only 8 percent of the overdose deaths in the city. The rest were due to fentanyl and heroin.Gavril Pasternak, a neuropharmacologist at the Memorial Sloan Kettering Cancer Center in New York, also warned in another letter about the consequences of cutting off access to opioids for pain patients. “While there is no denying the addiction issues and the horrible cost of life,” he wrote, “we need to have a balance and not forget those who need these medications.”“I can not keep waking up every day to pain and living through moments of a bit of lower pain but still stuck on my couch. Please let me live!”
