Each week, we read what's going on the world of science and bring three of the wildest findings straight to you. Scroll through for the latest:
Advertisement
Advertisement
Advertisement
Watch more from VICE:
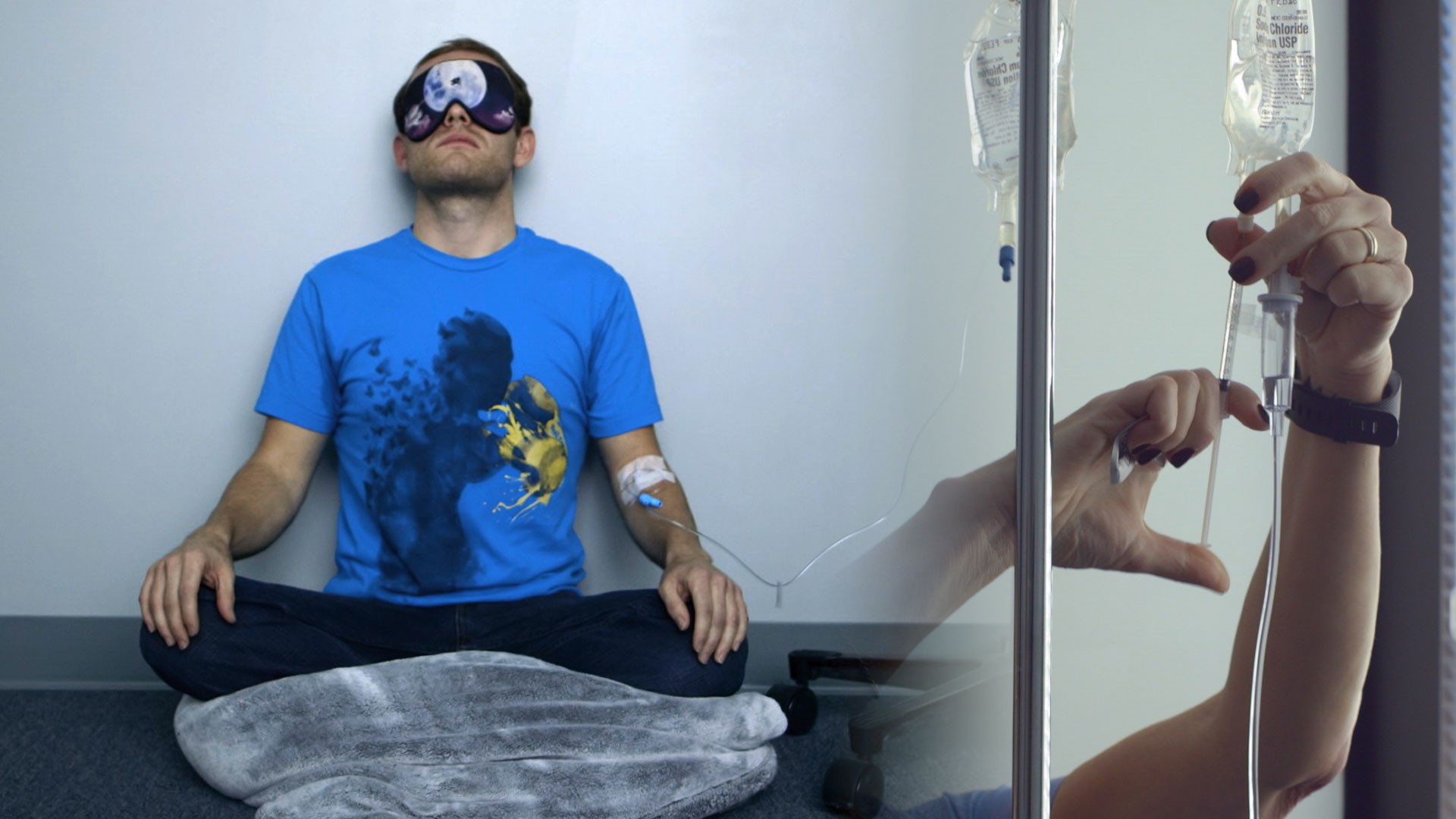
Just thinking about coffee could give you a slight buzzMy stomach decided about five years ago that it would not tolerate coffee anymore, and after a year of suffering from acid reflux, I dutifully switched to green tea. While I love my morning matcha, I do sometimes miss the buzzy high of a strong cup of coffee. A new study in Consciousness and Cognition suggests that perhaps I can still access some of that feeling—not by drinking coffee, but simply by thinking about it.Coffee is more than a beverage, it also has cultural beliefs and associations tied to it, says Eugene Chan, a senior lecturer in marketing at the Monash Business School in Australia and first author of the paper. “People also have lay beliefs about what coffee and other beverages do, and these lay beliefs, psychologists have shown, can produce their own effects,” Chan tells me.In the lab, they got people to think about either coffee or tea through a variety of tasks, like writing ads for either coffee or tea, or reading health articles about coffee or tea. The researchers then found the people who thought about coffee had higher levels of arousals, compared to the tea thinkers: they said they felt higher levels of arousal and their heart rates increased slightly. Because of this arousal, Chan says, their thinking styles were more focused and concentrated.More research needs to be done to see if the study’s effects can be replicated, or how it might change for different kinds of coffee (coffee versus a latte) or kinds of tea (black versus green), or people with different cultural backgrounds (where coffee might hold different meaning). But overall, the study adds to the evidence that the food and drinks we consume do more than provide nutrition, or interact with our bodies physically. “Mere exposure to or reminders of them can affect how we think,” the authors wrote.
Advertisement
Advertisement
Your weekly science and health reads
We are lucky to continue to have posthumous writings from the great Oliver Sacks, even years after his death. In this essay, Sacks muses about the calming effect of gardens—on himself and on people with neurological disorders.There's a gold-standard treatment for opioid addiction, one of America's top killers. What keeps treatment centers from using it? By Francie Dep in Pacific Standard.
For this piece, Dep spent months looking through state and federal data for centers in California that said they treated opioid addiction but didn’t use medication treatment.How a tiny endangered species put a man in prison. By Paige Blankenbuehler in High Country News.
“Trent’s underwear still floated in the water. The group huddled around for a closer look. In the pool, a single bright blue pupfish was also floating on the surface—dead.”The Helmet That ‘Resets’ Your Brain. By James Hamblin in The Atlantic.
It could help people with depression, but it also costs $12,000.Sign up for our newsletter to get the best of Tonic delivered to your inbox.
