Channey
Necrotizing fasciitis (or NF, the clinical term for flesh-eating bacteria) is an infection caused by swimming in infected water—and it’s very rare. Like, a few hundred cases a year rare. And yet, I personally know two people who just barely survived the disease. This summer, there have been headlines about the Russian musician who died from NF, and how a plane he was traveling on had to make an emergency landing because the smell of his rotting flesh sickened passengers. Currently, a New Jersey man is fighting for his life after catching NF while crabbing. He may lose all of his limbs.Alan Avery, an art gallery owner in Atlanta in his mid 50s, is one of my friends who survived a case of NF in 2016. He was on vacation with his husband at a beach in North Carolina when, he thinks, he might have scraped his stomach while surfing. A week later he had infected skin on his abdomen, but he and his doctor didn't think it was too serious. Within a few days, he began hallucinating (caused by sepsis, one of the complications of these types of infections).He describes sitting on the front porch watching his yard sculptures turn into 3-story giants walking down the street. His husband was away, and Avery called police in a state of hallucinatory paranoia. Luckily, they recognized he wasn't on drugs, but having some strange medical emergency that needed immediate attention. The doctors told him that a few more hours without treatment, and he would have died. “I was lucky they caught my infection early,” Avery says. “I had 11 surgeries. I spent a year in a wheelchair and walker. I'm lucky to be alive.”Most physicians will only see one case of NF in their career, and this means many doctors don't know to look for it and may misdiagnose it. While NF isn't something anyone should live in fear of because of infrequently it occurs, proper wound care is crucial.Many types of everyday bacteria can cause NF, says Colleen Kraft, an infectious disease doctor at Emory University. It isn’t necessarily mutant bacteria or exceedingly rare bacteria causing these infections. “NF is bacteria in the wrong place. When bacteria gets in the fascia—which is between the skin and the muscles—it’s like a superhighway for it to spread throughout the body,” Kraft tells me. “A lot of these bacteria are used to surviving in wet environments, so they spread like gangbusters when they get inside the fascia.”The usual suspects for NF infection are Group A Strep, E. Coli, Staph, and Vibrio (a particularly virulent strain found in saltwater). These bacteria are all around us all the time. Staph, for example, is commonly carried on the skin of otherwise healthy people. It’s only when a puncture on the skin allows it to get inside your body does it make you sick. The bacteria attack the fascia, completely killing it while moving on rapidly. Kraft says that the bacteria tries to push its way out as it kills soft tissue and continues to multiply, and because it is sandwiched between the skin and muscle it quickly spreads in the fascia “superhighway,” often unnoticed.She adds that it’s a fast moving infection, and one that can be hard to diagnose and the infection in the fascia could be very severe even though it looks okay from the outside. A key indicator that something is terribly wrong is pain that’s not in proportion to the wound—or “exquisite pain,” as Kraft calls it.
Watch this from VICE: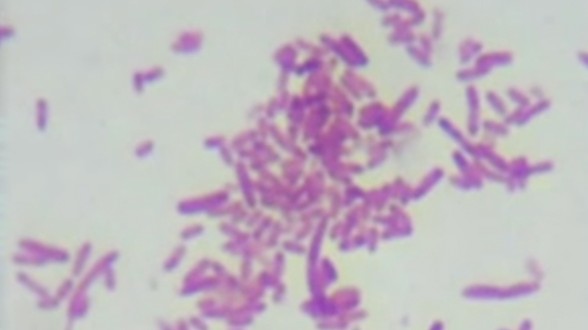
She says that treating NF can be a challenge because antibiotics can only stabilize you. NF-infected tissue has to be removed. Sometimes this means entire limbs have to be amputated because the bacteria has spread over an entire area. According to the CDC, 700-1200 Americans contract NF annually (and a fourth of these people have died from it), while the organization warns that the actual numbers are likely higher, since many cases go unreported. The CDC tracks infections caused by Group A Strep, the most common source of NF infections (the strep can evolve, apparently).This gap in data is especially frightening, when you consider that these many other strains of bacteria like Vibrio, E. coli, and Aeromonas hydrophila thrive in water such as lakes, rivers, saltwater, pools, and hot tubs. These bacteria are very dangerous if they get below the skin and infect human tissue. Last year, at least two people died from NF after contracting it from dirty floodwaters in Hurricane Harvey (if NF goes untreated, it’s fatal). You don't even have to be swimming in the water to be in contact with the bacteria—it’s believed that a California father of two contracted NF through abrasions on his hand while handling fish he'd caught in water that had the bacteria.Candice Hoffman, a CDC spokesperson, recommends that people should stay out of a lake, river, or beach, if it is closed or an advisory is posted for high bacterial levels or other conditions such as sewage spills or harmful algal blooms. They also advise to stay away with fish or other animals in or near the water are dead or if water is discolored, smelly, foamy, or scummy.Fortunately, most major recreational bodies of water are tested by local environmental protection agencies, which issue public advisories when bacteria levels exceed safe thresholds. Recently, the New Jersey Department of Environmental protection issued an advisory for 47 beaches having unsafe levels of fecal bacteria. A week later, two were closed completely after failing another bacteria test.This was the result of storm water from very heavy and widespread rainfall, which brings higher levels of bacteria, says Larry Hajna, a press officer for New Jersey Department of Environmental Protection. “The beaches were re-tested and all but two passed, meaning advisories were lifted. The two beaches that were closed were river beaches in Ocean County that did not pass the re-test. They passed the next test and were opened.”The beaches with the highest levels of bacteria tend to have brackish water—that is, salt water mixing with freshwater coming in from a river. Hanja says whatever is upstream is washed out to the beach (including animal waste), which can present a bacterial swimming hazard. It also bears repeating that saltwater—in a pool or ocean—can carry harmful bacteria that can result in NF.Hoffman advises that protection is as simple as treating a wound correctly if you end up with one. “Prompt first aid can help heal small wounds and help prevent infection. If possible, wash your hands with soap and water before and after taking care of your wound,” she says.When you go swimming this summer, it also can’t hurt to pack these four things along with your bathing suit and sunscreen, because they constitute a simple wound care kit: bottled water, antibacterial soap, hydrogen peroxide or rubbing alcohol, and a waterproof bandage.Any foreign matter, like dirt or sand, needs to be thoroughly washed out of the wound. Next, gently cleanse the area with antibacterial soap and again wash clean. A final rinse of alcohol or peroxide will further sanitize the site. Unfortunately, you cannot slap on a waterproof bandage and hop back in the water, as that could trap in bacteria and make an infection more likely. Waterproof bandages are important to cover existing wounds before going swimming.Immediacy of wound care is important, Hoffman says, because these bacteria work very fast. If you scrape, cut, or even nick your skin while swimming, it needs to be cleaned and bandaged as soon as possible—not later, not when you get back to the house, not after a few more drinks. Immediate and proper wound care greatly reduces the chance of NF. Just as you would check for ticks after hiking in the woods, you should also check yourself for abrasions after swimming—even in a swimming pool.In Metro Atlanta, where I live, is the Chattahoochee River. One of the most popular summertime fun trips for Atlantans is to “Shoot the Hooch”—which is to go down the river in tubes with all your friends and many coolers of beer. I used to do this at least once every summer in epic flotillas of friends. Dotted along the Hooch are cow farms, which means all those cow patties are getting washed into the river after a big rain. As the Hooch moves from the suburbs into the city, you see apartment complexes along it, which means shit from the dog park, leaking car oil, dumpster juice, and whatever other urban detritus is also getting washed into the river.“You might as well be swimming in sewage,” Kraft says to me about my Hooch excursions. She won’t let her kids swim in the Hooch. Recently she had a friend who got a cut while Shooting the Hooch, and the friend wanted to know how alarmed to be. Kraft reminded her friend that contracting NF is unlikely, but to monitor the cut and go to the doctor if starts to look bad. She also says that most healthy people should be okay to swim in these types of waters. NF infections are more common when people have other risk factors such as diabetes, immunodeficiencies, have had a recent infection, or are elderly.So I should be fine. Still, though, I’m always going to check the bacteria report for wherever I go swimming, and make sure to practice proper wound care if I get cut, regardless of how many beers in I am.Sign up for our newsletter to get the best of Tonic delivered to your inbox.
Advertisement
What causes Necrotizing Fasciitis?
Advertisement
Watch this from VICE:

She says that treating NF can be a challenge because antibiotics can only stabilize you. NF-infected tissue has to be removed. Sometimes this means entire limbs have to be amputated because the bacteria has spread over an entire area. According to the CDC, 700-1200 Americans contract NF annually (and a fourth of these people have died from it), while the organization warns that the actual numbers are likely higher, since many cases go unreported. The CDC tracks infections caused by Group A Strep, the most common source of NF infections (the strep can evolve, apparently).This gap in data is especially frightening, when you consider that these many other strains of bacteria like Vibrio, E. coli, and Aeromonas hydrophila thrive in water such as lakes, rivers, saltwater, pools, and hot tubs. These bacteria are very dangerous if they get below the skin and infect human tissue. Last year, at least two people died from NF after contracting it from dirty floodwaters in Hurricane Harvey (if NF goes untreated, it’s fatal). You don't even have to be swimming in the water to be in contact with the bacteria—it’s believed that a California father of two contracted NF through abrasions on his hand while handling fish he'd caught in water that had the bacteria.
Advertisement
How do you know what waters to avoid?
Advertisement
How can you protect yourself from flesh-eating bacteria?
Advertisement