Annabel Wright was 15 when she killed herself last spring. She loved horse riding and dogs, and was the only daughter of Helen and Simon Wright. She had also just been prescribed a course of Roaccutane, a potent medication used to clear nodular, cystic acne that has an unconfirmed link to depression.
While the cause of Annabel’s death is yet to be confirmed, her parents blame the drug. At the end of 2019, the Guardian reported that ten out 12 deaths connected to Roaccutane were by suicide – the highest since records began in 1983.
Videos by VICE
The safety of Roaccutane, a brand name for the drug isotretinoin, has been debated in the House of Commons four times in the past decade, with the last government-funded review taking place in 2014. The Medicines and Health products Regulatory Agency (MHRA) concluded that the data was “insufficient” in establishing a link between Roaccutane and depression, but that “an association could also not be ruled out.” Instead, they insisted that the current warnings on Roaccutane’s product information, added in 1998, should be emphasised.
But for 27-year-old Bethany Simpson, the written warnings didn’t make clear the long-term impact Roaccutane would have on her mental health. She was 15 when her dermatologist prescribed her the medication. “I still have issues now,” she tells me over the phone. “I’m pretty convinced [Roaccutane] was a definite cause.”
Half way through the six-month course, Simpson’s mood began to dip significantly, leading to arguments with those closest to her. “I remember being like, ‘I can’t understand why I feel like this’ because especially towards the end [of the prescription], my skin started to clear up and I was like, ‘I should feel way happier’ but I definitely didn’t.”
Simpson also felt that her depression wasn’t being taken seriously by the medical staff who prescribed Roaccutane. “There was never a full check-in,” she says. “[The nurse] said, ‘How’s your mood?’ and I said, ‘Fine.’ And that was the end of that, really.”
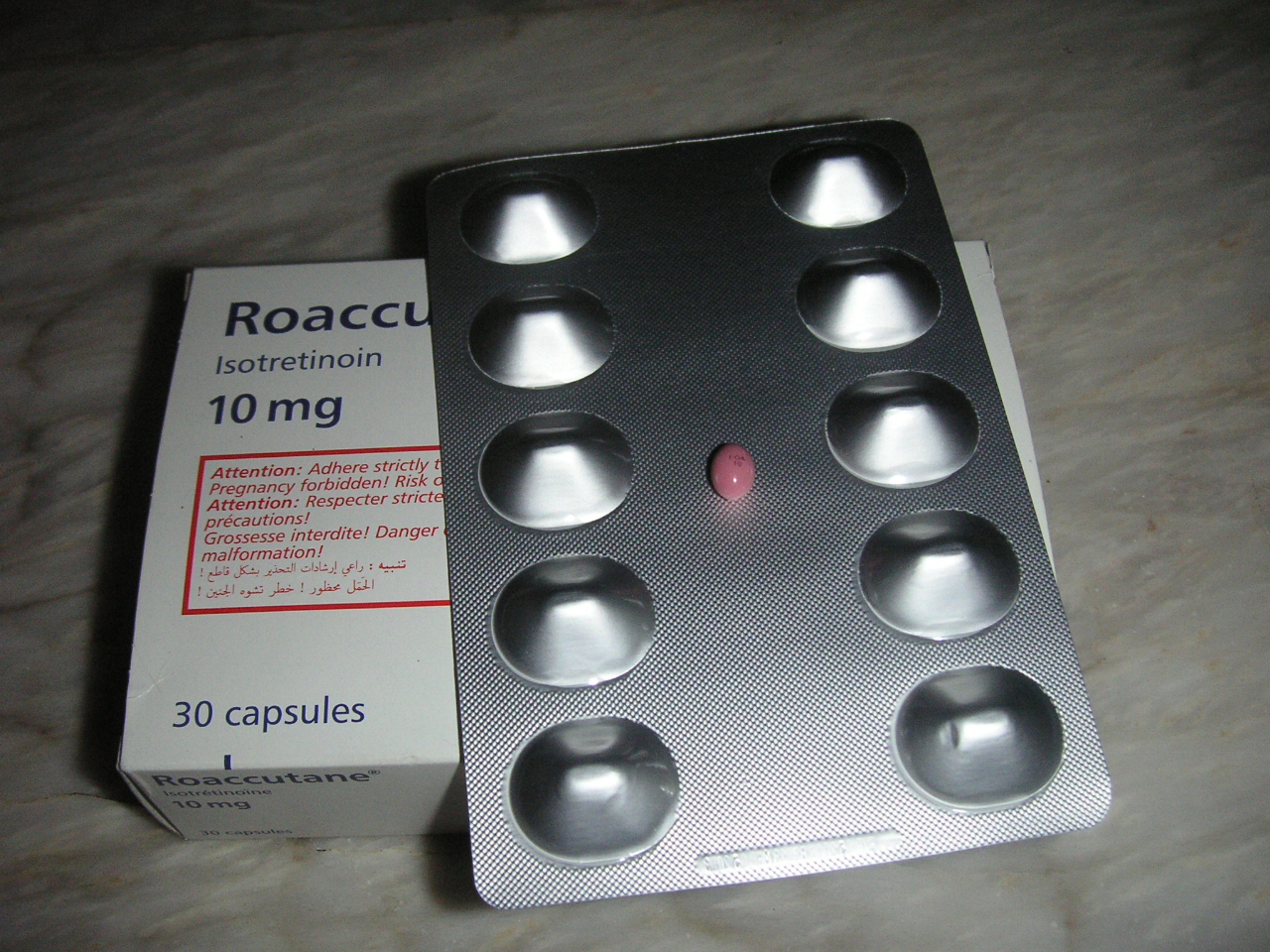
Roche, the pharmaceutical company that manufacturers Roaccutane, says that it takes the safety of all its medications seriously. A spokesperson told me: “It is vital that patients are fully informed as to what to expect when they take it and that they are monitored closely to ensure they get the ongoing care they need.”
In the 2014 review, before any data on the psychiatric effects of Roaccutane is discussed, the MHRA takes care to explore the pre-existing link between acne and depression. It’s a double-edged sword: while this defence can’t account for patients like Simpson, whose depression persisted after her skin healed, the anxiety and lack of self-esteem felt by acne sufferers is worth acknowledging.
I was first prescribed Roaccutane for my acne at 15, and then again at 22. For me, the meteoritic rise of skincare as a fashionable hobby exaggerated my poor mental health. In the past decade, skincare has exploded into the mainstream, gobbling up nearly 60 percent of the global cosmetic market growth, with the industry projected to reach £134 billion by 2025. Reddit’s “r/SkincareAddiction” gets more than 1,000 posts a day. During my second course of Roaccutane medication, I remember watching girls no older than 13, with glassy, prepubescent complexions queue to buy £50 jars of face mask at my local Urban Outfitters.
This shame felt by many acne sufferers is only intensified by the current trend for skincare as fashion. Although Annabel Wright’s acne was classified as non-severe, her dermatologist suggested Roaccutane as the best method to prohibit any scarring. “And to Annabel,” her mother told Channel 4 in October, “that was everything.”
So, why is Roaccutane, a drug with climbing suicide rates, still taken by 30,000 people every year? In comparison, weight-loss “wonder drug” Acomplia was pulled from the UK market in 2008 after being linked to five suicides in a trial of 36,000 patients. Unlike the MHRA’s 2014 review of Roaccutane, there was no mention of the pre-existing relationship between obesity and depression in the European Medicines Agency’s official press release.
Glen Hamilton, 40, who was prescribed Roaccutane in 2007, points out that there are not many alternative acne treatment options. “There weren’t any other drugs being suggested as a solution,” he tells me. “[My dermatologist] did say to me that he would take it himself, but that he was a risk taker. And that’s the way it was positioned to me.”
The reality is that the social stigma surrounding acne runs deep. Just like Hamilton’s dermatologist, society tells us that clear skin is always worth the risk.
Hamilton made the decision to stop taking the medication just six weeks into the course, but within those six weeks already so much had changed. “I just remember I left my job, I struggled to work and I just felt incredibly down. Like the world was going to end.”
Dr. Jibu Varghese, a consultant dermatologist in the south west of England, says that the percentage of patients who experience such side effects are significantly low. Despite Roaccutane’s product information instructing patients to alert their doctor to any previous cases of mental illness, Dr. Varghese tells me this is not a contraindication for a Roaccutane prescription. “I’ve got a patient who had postnatal depression,” he says, “now she’s completed her course safely.”
But for many, opening up about mental health is still a challenge. David Kochanowicz, 20, says that the lack of emphasis professionals placed on Roaccutane’s potential mental health side effects made him believe the depression he was experiencing was “a separate issue.”
Kochanowicz says: “The only side effects they talked about were cosmetic, so dry lips, skin, pregnancy in women and what not. Mental illness wasn’t really something that was raised.”
Like many other Roaccutane patients, Kochanowicz’s experience of the medication hinged on his ability to fill in the gaps of NHS support. Due to the long wait list to see a therapist, he relied heavily on the helpline provided by mental health charity Campaign Against Living Miserably.
A new inquiry into Roaccutane’s safety will be conducted by the Isotretinoin Expert Working Group, with the first meeting set to be “as early as possible in 2020”. Rather than an outright ban of the drug, Hamilton believes that closer psychiatric monitoring, more comprehensive warnings and a better support system for patients is needed.
“That would be the most sensible route,” he concludes, “just being aware it can have really serious side effects in terms of mental health and then giving channels to communicate and get support if they need it. It’s that life changing stuff.”
More
From VICE
-

Photo: Lajst / Getty Images -

Photo: The Good Brigade / Getty Images -

Photo: kelly bowden / Getty Images -

Photo: Rawpixel / Getty Images
