Some 16 million Americans had at least one major depressive episode in the past year and approximately 29 million Americans are taking antidepressants. While some may look at these statistics and see a growing mental health crisis, pharmaceutical companies see dollar signs.
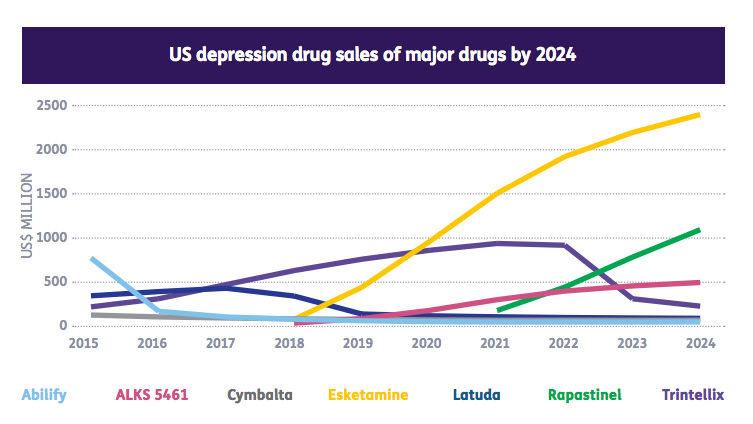
According to a new report [pdf] by the pharmaceutical data analysis firm Informa Pharma Intelligence, current market value for depression medications in the US is $4.6 billion a year and expected to grow to $7.3 billion by 2024. To capitalize on this growing demand, a whole new suite of depression drugs are being pushed through the Food and Drug Administration approval process—and according to Informa, this new class of depression meds are going to “upend the overall market.”
Videos by VICE
The new drug classes, which include ketamine- and opioid-based drugs, will drive most of the increase in sales, accounting for $4.15 billion by 2024. That’s almost the size of the market now.
For the most part, the antidepressants being sold today are either selective serotonin reuptake inhibitors (like Prozac or Zoloft), or the newer serotonin-norepinephrine reuptake inhibitors (like Pristiq or Efexor). Both SSRIs and SNRIs affect serotonin neurotransmitters in your brain by blocking the serotonin reuptake and trapping the mood-stabilizing chemical in the gap between neurons for longer than normal. SNRI’s are like SSRI’s, but they also regulate the release of norepinephrine, a brain chemical that’s largely responsible for mobilizing the body for action much in the same way as its cousin epinephrine—you know that one as adrenaline.
Since lower-than-normal serotonin levels have been linked to depression, the thinking was that increasing access to this chemical could alleviate symptoms of depression. But these types of medications only work in about 60 percent of depression patients, and the link between low serotonin levels and depression is much more dubious than previously thought.
Watch more from Tonic:
The new classes of antidepressants—such as the nasal spray esketamine being developed by a Johnson & Johnson subsidiary, or the opioid-based ALKS5461 developed by Alkermes—target NMDA receptors. These receptors regulate the concentrations of the glutamate neurotransmitter in the brain, and recent research has shown that higher levels of glutamate are linked with major depression. So drugs that target NMDA receptors and regulate the chemical might help with depression. While both of these medications are undergoing FDA clinical trials for approval as antidepressants, the Informa report warns they also carry a risk for abuse or addiction.
Esketamine is the sibling of ketamine, which was recognized as a good candidate for an antidepressant more than a decade ago. But psychiatrists such as James Murrough, an assistant professor of psychiatry at Icahn School of Medicine at Mt. Sinai, caution against rushing to use ketamine as an antidepressant. This is also the view of an American Psychiatric Association research task force that recently published a report in JAMA Psychiatry arguing that ketamine isn’t quite ready for widespread use as an antidepressant.
“We haven’t had large-scale trials [for ketamine],” Murrough told NPR earlier this year. “We don’t know how much or how often it should be given for it to be effective or safe.”
Although ketamine and esketamine are similar insofar as they target the neurotransmitter glutamate , the latter does appear to have some crucial differences such as decreased dissociative properties—that is, when people are awake but totally detached from their surroundings—compared to ketamine. In fact, esketamine faired so well in its clinical trials that last year the FDA designated it as a “breakthrough therapy” for depression with an imminent risk of suicide. Earning this status expedites the approval process on the grounds that “preliminary clinical evidence indicates that the drug may demonstrate substantial improvement over available therapy.” In the case of esketamine, the drug is being developed as a therapeutic class specifically designed to have a rapid onset in their effects.
“The need for new treatments is great because only one-third to 45 percent of depressed patients attain remission with current antidepressants or psychotherapy,” Charles Nemeroff, a psychiatrist at the University of Miami specializing in depression, told me. “Depression is associated with a high risk for suicide, the tenth leading cause of death in the US and the only one that continues to increase.”
The hope is that the new suite of antidepressants will work for patients who have not responded to other types of treatment for depression, as well as provide a fast-acting relief for those at the greatest risk of suicide.
Daniel Chancellor, the lead analyst at Informa, told Tonic that Johnson & Johnson will likely be able to command a high price for esketamine due to its fast-acting effects, although it will likely only be available to depression patients who’ve been unresponsive to other drugs.
“There’s no precedent for drugs like this in depression,” Chancellor said. “So there’s a bit of uncertainty for how J&J will price it. They’re going for a niche, but a relatively large niche, so they’ll likely try to extract as much value out of it as possible.”
According to Nemeroff, esketamine, which lasts for 1 to 7 days at most, the drug is being studied as “an adjunct to antidepressant treatment, not as a monotherapy.” In other words, the fast-acting antidepressant would be administered on an as-needed basis in addition to other treatments, but would not be used as the sole treatment for depression.
However Nemeroff also noted that that ketamine is “a major drug of abuse and there is little in the way of long-term data with either ketamine or esketamine.” More troubling is that “many patients who receive ketamine have not yet received other FDA-approved treatments for depression such as repetitive transcranial magnetic stimulation or a variety of medication combinations, not to mention evidence-based psychotherapy such as [cognitive behavioral therapy].”
“In the end, we must be driven by data,” Nemeroff told me in an email. “If once a week esketamine or another agent is able to help severe depression without serious side effects or drug abuse liability, then it would be a great addition to our armamentarium.”
As for ALKS5461, its potential as an effective antidepressant is less certain. In the first two of three phase III studies—the clinical trial phase in the FDA approval process involving at least 300 patients—the drug failed to meet primary endpoints showing its efficacy. In other words, it failed to be more effective than a placebo.
The shocking clinical results resulted in nearly $4 billion being wiped out from the company in 2016 as investors wrung their hands wondering if the drug was even effective. Late last year, ALKS5461 had its first successful Phase III trial and recently launched a late-stage Phase III study to investigate its possible side effects.
As an opioid-based treatment in a nation reeling from an opioid addiction crisis, ALKS5461 was already fighting an uphill battle to be accepted as a legitimate treatment before its less-than-stellar results in the clinical trials. Assuming it manages to get through the FDA approval process, the Informa report predicts the drug will still be “greatly debated and scrutinized” due to its high risk for abuse and addiction.
Still, Chancellor was optimistic that ALKS5461 would get approved, based on the FDA’s historic leniency when it comes to approving antidepressants.
“There’s a strong precedent with the FDA for approving depression drugs even if they have been involved in failed clinical trials,” Chancellor said. “Depression is quite a difficult space to do clinical trials in because the placebo effect is quite strong. There are quite a few drugs that have gone before the FDA with negative studies alongside positive studies, and the FDA has approved them.”
Despite their risks, the Informa report says both ALKS5461 and esketamine will be approved for sale in the US by July 2018. The latter is expected to have initial sales of around $45 million in 2018, even though it is likely to be classified as a Schedule III controlled substance.
The Informa report also polled 238 physicians and psychiatrists around the world who treat patients with depression, and found that nearly half of their drug-treated major depressive disorder patients were unresponsive to initial antidepressants and had to go through a “trial and error process in the quest for finding a suitable therapy.” Moreover, the health care professionals reported that only 59 to 79 percent of their patients adhere to their antidepressant due to intolerable side effects or ineffectiveness of the treatment.
Clearly there are problems with depression therapy—the question is whether esketamine and ALKS5461 are the best way to approach them.
Read This Next: This Psychedelic Drug Targets Addiction and Depression
More
From VICE
-

Lettuce (Credit: Sam Silkworth) -

Screenshot: Pokemon Go -

Clara Balzary -

Screenshot: NetEase