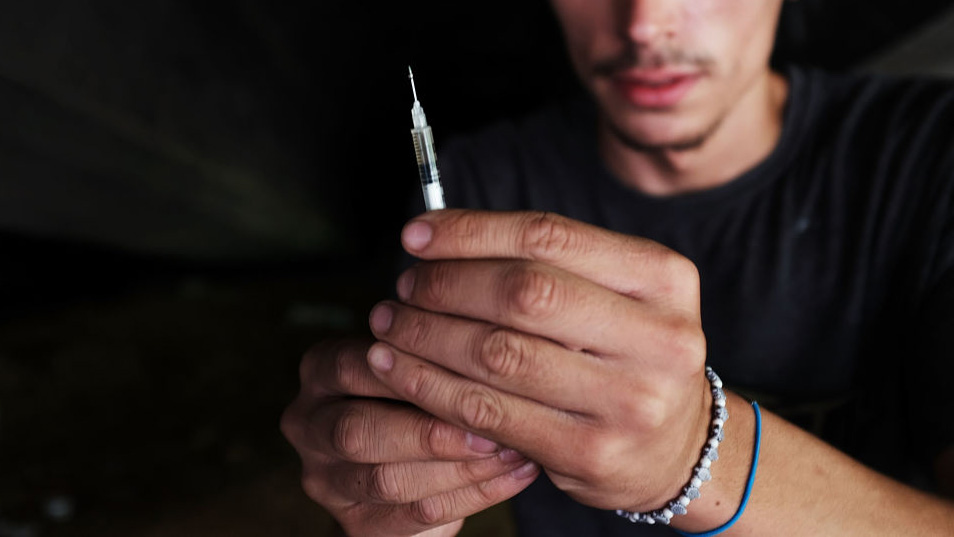
In an undisclosed location in the US, a social services agency has secretly overseen more than 2,500 injections by around 100 people who take drugs—in an effort to fight the overdose crisis. The underground “supervised injection facility” (SIF) has been in operation since 2014, and is open for four to six hours a day, five days a week, according to a new study published in the American Journal of Preventive Medicine. It has seen no deaths, no apparent neighborhood problems, and the onsite reversal of four overdoses. As a condition of their research, the authors of the paper did not disclose the facility’s location as it’s unsanctioned and potentially illegal.
While such facilities are controversial in the US, they have operated for years in 66 cities worldwide—in Canada, Australia, Spain, Denmark, Norway, France, Germany, Luxembourg, the Netherlands and Switzerland. Thousands of injections have been observed at these sites—and no one has ever died of an overdose at one. Meanwhile, research finds that, contrary to fears, SIFs actually increase drug treatment enrollment, reduce drug use, cut overdose mortality, and slow the spread of bloodborne diseases like HIV and hepatitis. Cities like San Francisco, Ithaca, New York, and New York City are pursuing the idea and the county that includes Seattle has already approved opening two facilities.
Videos by VICE
Why do sites that apparently condone drug injection actually encourage recovery? The paradox dissolves if you understand the real drivers of unsafe drug use and addiction: stigma, criminalization, mental illness, despair, and trauma. When people with addiction are provided with a safe, caring, and nonjudgmental atmosphere, they can slow down and engage in practices that allow safer injection, they have better access to clean equipment, and basically, time to think.

Moreover, when you find a corner of the world that doesn’t demand that you change before you’re deemed worthy of saving, which doesn’t focus on your flaws and actually tries to provide you with what you need, as you are, right now, you tend to be more open to suggestion. When you see that other people value you, you start valuing yourself more—and when you recognize that staff want to help you attain the goals that matter to you, you start to think differently.
Often, over time, this leads to reduced intensity of drug use—and to treatment that helps ease mental illness and other trauma, which tends to be what pushes people to compulsively seek chemical relief. Once people feel more comfortable in their own skin, they tend to become more ready to shed addictions.
Sadly, in Trump’s America, we still don’t understand these principles of harm reduction—even though, for example, we’ve had the data for decades to show that all of this is true regarding syringe exchange programs. In New York—the epicenter of the HIV epidemic in IV drug users—at least 50 percent of people who injected drugs were infected by 1990. As needle exchange was introduced, along with other measures to increase clean needle access and expansion of medication treatment, that rate fell. By 2012, just 3 percent were infected. And needle exchanges helped bring people into treatment and recovery: they didn’t prolong drug use or encourage new users to start injecting. There’s no reason to see SIFs any differently.
But rather than create safer injection sites and declare a state of emergency to allow expansion of access to medication treatment with methadone and buprenorphine—the only two treatments, which, when used long term, can cut the death rate in half—President Trump has called for more prosecution of drug crimes. That approach has never actually been associated with reduced drug use or overdose. Nor does his call try to scare youth away from opioids by telling them that they are “No good, really bad for you in every way,” have any evidence to support it.
If we want evidence-based drug policy, we’re going to have to fight for it.
Read This Next: Doctors Should Be Using Heroin to Treat Addiction
More
From VICE
-

Photo: drante / Getty Images -

Photo: dbvirago / Getty Images -

Credit: DuckDuckGo -

Photo: Oleg Breslavtsev / Getty Images